You are on call in the middle of a case in OR. You are paged by CCU to attend to a pre-arrest STAT. You run up to the CCU, to find the patient on BiPAP, with RT, RNs, the CCU fellow and resident present. The quick history you get from the fellow is the patient was planned for a TAVI (transcatheter aortic valve implantation) earlier in the week, but was cancelled because he had CHF and was admitted to CCU for diuresis. About 30min before you were paged, he acutely desaturated to SpO2 65%, ddx was flash pulmonary edema or aspiration.
On arrival at the bedside...
The CCU fellow is suggesting that you give the patient 10-15 mins trial of BiPAP to see if hypoxia will improve.
2) Breathing – the work of breathing itself is metabolically high, and taking over respiration with mechanical support will conserve that oxygen for other vital tissues. He will not improve on BiPAP if the cause of the hypoxia is aspiration.
3) Circulation – remember the main disease is critical aortic stenosis. The hemodynamic goals with AS are normal sinus rhythm (maximize LV filling with atrial kick), slow-normal HR (maximize diastolic filling and LV perfusion time), high afterload (need higher myocardial perfusion pressure) and adequate preload (may need higher LAP to fill stiff/hypertrophied LV). Lack of beat-to-beat invasive BP monitoring, and lack of adequate IV access. Hypoxia and hypercarbia will also increase pulmonary vascular resistance through hypoxic pulmonary vasoconstriction reflexes, and will further impede forward flow.
An arterial blood gas result that was drawn 15 mins ago comes back as pH 7.19 / pCO2 123 / pO2 44 / Bicarb 45 / Base excess 12.
1) Continue BiPAP – probably not the best option because of aforementioned reasons and hypercarbic/hypoxic respiratory failure
2) Optimize hemodynamics with cardioversion or rate controlling agents – may or may not stay in sinus. The patient was actually in chronic AF, and thus cardioversion would likely have failed.
3) Intubate.
So you decide to intubate the patient. What is your plan for management of their airway?
1) First attempted to perform deep suction with the RT to try to clear out any mucus plugging that may have been causing the decreased air entry I heard on auscultation. Unfortunately, we did not aspirate much and the patient’s SpO2 did not tolerate lack of PPV very well.
2) I performed manually-assisted BMV in sync with patient’s own respirations as well as intermittent PPV. The highest SpO2 I could achieve during the ~60s before all my intubation equipment was set up (suction, ETT, scope) was ~76-78%, therefore I decided to proceed.
3) I asked the RN to push phenylephrine 100mcg IV – a total of ~500mcg was given peri-intubation. Direct look with Mac 3 with no sedation/meds/topicalization. Rationale was patient was critically ill and already obtunded from hypoxia/hypercarbia. Gr 2 view with lots of pink froth coming up underneath the epiglottis. Suctioning did not clear it up – constant stream. Styleted ETT was placed while patient was spontaneously breathing. His cords tried to close on the ETT, which was advanced during inspiration, and stylet was removed 1/3-1/2 way and the rest of the ETT was advanced gently through. Immediately it was filled with pink sputum and this was suctioned with inline suction.
4) We attached the patient to the vent with a starting PEEP of 5 to see if his hemodynamics would tolerate it. Over the next 5-10mins his SpO2 improved to 88%, which were the highest they’d been in a while.
I stayed for a while longer while the CCU fellow inserted a femoral line and started a dopamine infusion.
Dopamine was probably not a good choice because of it’s effects on increasing heart rate and pulmonary vascular resistance (PVR). Pursuant to the SOAP-II trial, norepi might have been a better choice since it increases systemic vascular resistance (SVR) more than dopamine, and does not have such a great effect on HR. It does, however, also increase PVR.
Vasopressin would probably have been my first-line pressor of choice. It increases SVR without increasing PVR or HR. The goal is to improve myocardial perfusion pressure and not overload the RV.
Eventually the patient died later that night on three pressors and after a family discussion regarding futility of further escalation of care. At the time, I had noticed very deep T waves on the ECG monitor.
This was his preintubation CXR, which was not available to be viewed until later:
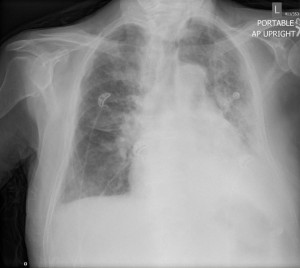
And this was the postintubation CXR:
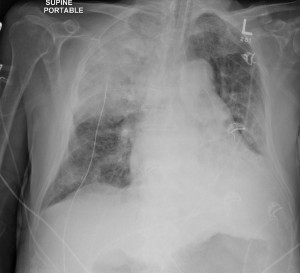
What I didn’t know until I reviewed the chart afterwards, was that his echo had showed elevated RVSP in the 60s and decreased LV function, both indicative of severe AS and decompensated LV function, causing backup of pressure into the pulmonary vasculature and causing pulmonary hypertension.
Here is a video depicting why tachycardia is so bad for severe aortic stenosis:
Paced tachycardia in critical aortic stenosis from Taylor Zhou on Vimeo.
1) Hypoxia and hypercarbia worsen pulmonary vascular resistance
2) Atrial fibrillation/tachycardia/hypotension bad for aortic stenosis
3) Obtunded, critically ill patients may not need any medications for intubation
4) They will get worse after intubating and initiating PPV before they get better
5) Vasopressin perhaps the best first choice pressor for patients with AS or pulmonary hypertension/RV failure




