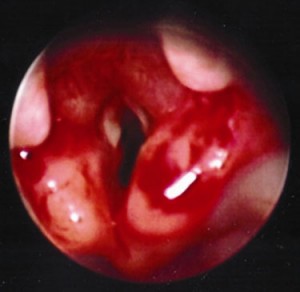
Dr. Levitan recently posted an excellent article on four tips to video laryngoscopy. Here are my summary and thoughts:
- Suctioning and epiglottoscopy:
A clean, clear pathway is crucial for successful video/indirect laryngoscopy. Blood/vomitus/copious secretions will complicate indirect laryngoscopy immensely. For elective/semi-elective situations, a antisialologue (e.g. glycopyrrolate 0.4-0.8mg IV) can be used, if tachycardia can be tolerated. For emergency situations, very bloody airways or profuse, active vomiting, two working suctions are key.
The first step is to identify recognizable structures such as the epiglottis, especially when airway anatomy may be very different in difficult airways. Even with direct laryngoscopy, find the epiglottis first and then move the blade tip into the vallecula. As long as you can identify the epiglottis, even if you cannot identify a normal glottic opening, you can try to pass a bougie in the general direction under the epiglottis. - Lift the mandible to expand the viewing space:
I find the benefit with using Glidescope vs. direct is using less force lifting the jaw. The curve of the blade itself is sometimes enough to create room to see the glottis, and sometimes lifting can obscure your view or pull the glottic apparatus away from the centre of the screen, thus artificially making the glottis more “anterior”. When passing the Glidescope blade, just follow the curve of the blade and try not to do any lifting at first. - Tilt the optics away from the target (toward the ET tube):
The main point is to try to get the glottic opening in the upper 1/2 to 1/3 of the screen, to allow visualization of your ETT approaching the arytenoids. - Two stage tube delivery:
Dr. Levitan’s suggestion of “STOP, POP, and DROP” is essentially the way that I intubate spontaneously breathing patients who often get “laryngospasm” when trying to insert the ETT through the cords. Vocal cord closure is to be expected in a spontaneously breathing patient with intact airway reflexes, but this can cause significant problems for users who are not familiar intubating this way. The key point to getting the tube through is to time the advancement with the patient’s inspiration, since this will open the cords. If the patient is too obtunded and cannot control their airway reflexes, they may go into full laryngospasm and attempt to breathe against a closed glottis (which can cause negative pressure pulmonary edema). A light sedated or purely topicalized patient should not do this. Once the tip of the ETT is in, the cords will close down around it and the patient will start to cough. This is contraindicated if the patient was actively vomiting / raised ICP / or any other reason why they should not cough or buck the tube (e.g. globe rupture). At this point, disengage the stylet partly and advance the ETT.
Another tip for possible “anterior larynxes” on Glidescope is to add a very acute curve on the stylet. This may cause the ETT tip to go anterior to the glottic opening, but upon partial withdrawal of the stylet, the natural curve of the ETT will bend posteriorly.
This was a very good article from Dr. Levitan which helps to highlight some of the common obstacles encountered with indirect laryngoscopy and how to troubleshoot them. A frequent complaint I hear from emerg or medicine residents on ICU is that their senior or supervising person steps in too quickly if they run into trouble, and they don’t get the opportunity to troubleshoot themselves. I still believe a certain level of proficiency with ‘normal’ airways in controlled situations is necessary before attempting to troubleshoot in difficult situations (I include ICU, traumas, and any emergency airway in which there is little preparation time or ability to examine the airway).
Dr. Levitan is an emergency medicine physician, and also founder of Airway Cam Technologies Inc. Image credit: Lurie Children’s Hospital.